Real-World Use of Open Source Artificial Pancreas Systems – Poster Presented at American Diabetes Association Scientific Sessions
The OpenAPS community submitted an abstract that was accepted for a poster presentation at the American Diabetes Association’s Scientific Sessions meeting. The embargo lifted this morning, so you can read the abstract here or read below for the content from the poster to get insight from outcomes observed by those individuals who self-built hybrid closed loop artificial pancreases and insights we hope the healthcare provider community and diabetes community can learn from.
—
BACKGROUND:
Over a period of 16 months, over 81 patients (as of June 8, 2016) worldwide have built Artificial Pancreas Systems (APS) with off-label use of existing insulin pumps, continuous glucose monitors (CGM), and open source software (known as OpenAPS).
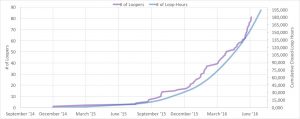
The patients have been using these systems outside of any clinical trial setting for more than 150,000 total hours.
OpenAPS is designed to be, and has been, far safer than standard pump/CGM therapy, as measured by duration of hypoglycemia and hyperglycemia, with no reports of severe hypo or hyperglycemic events. It has allowed patients and caregivers remarkable improvements in quality of life due to increased time in range, uninterrupted sleep, and peace of mind.
COMPONENTS OF AN OPENAPS SYSTEM:
- Continuous glucose monitor
- Older model insulin pump that allows user to remotely set temporary basal rates
- A “controller” device (small computer like Raspberry Pi or Intel Edison)
- Battery or power source for the controller
- A “translator” device to read/write to the pump (Carelink USB stick or TI radio stick, etc.)
SELF-REPORTED OUTCOMES:
At the time of the abstract submission, 18 users (out of 40 users total using the system at the time) shared and self-reported their data and experiences from using the system.
OpenAPS users (18 respondents, 67% male / 33% female, 61% adults / 39% children, median 27 years old (SD 14.5 years), 15 years with diabetes (SD 11.7 years), 10 years on pump therapy (SD 3.6 years), 3 years on CGM (SD 2.5 years)) were surveyed on quantitative and qualitative measures of their experience using their self-built APS. While using OpenAPS, self-reported outcome measures showed median HbA1c dropped from 7.1% (SD 0.8%) to 6.2% (SD 0.5%), and median percent time in range (80-180 mg/dL) increased from 58% (SD 14%) to 81% (SD 8%). All but one respondent reported some improvement in sleep quality, and 56% reported a large improvement.
Users caution that DIY APS implementations require significant effort to build and maintain, and pointed out that these systems cannot be considered a “technological cure,” but were extremely satisfied with the “life changing” improvements associated with using an APS.
DISCUSSION:
- Many users reported their health care providers (HCP) as being supportive, but some expressed disappointment at lack of interest from their HCP.
- These experiences are instructive for what patients can expect from commercial APS when they become widely available, and can help HCPs be prepared to set patients’ expectations properly when discussing or recommending an APS.
QUESTIONS FOR HCPs:
- Artificial pancreas systems are already here. One of your patients may already be building one. Would you know it if they are? Do you discuss with your patients which tools they choose to use to help manage their diabetes?
- APS are a powerful tool, but not a cure. Patients and HCPs will each still need to do a lot of work to use them effectively to improve diabetes management.
- Patients and HCPs must educate themselves and each other on how APS can be used effectively in daily life.
—
You can find out more about OpenAPS on OpenAPS.org, from the reference design to frequently asked questions (such as what hardware is needed and where the code and documentation can be found) and links to news articles on OpenAPS community.
Thank you for your efforts
Thank you form our hearts
Thank you because you try to do something they telling us “it’s not now … maybe after 10 years”
Thank you Dana my darling
Me and Sarah mother
From our hearts
THANK YOU DANA
While the automatic feature of any APS makes glucose control easy, it is also expensive. The most important component of an APS is the CGM, and not the pump, which can be replaced with the same syringes and pens as before (using TID NPH and Regular or Fast insulin at dawn for the Basal dose).
For a responsible user, what is really needed is the controller device to provide Bolus insulin quantity and timing info, which in a manual system could be a smartphone App. I suspect manual operation could be even better than automatic, because the APS needs to wait over a half hour to know the user has eaten, and even then doesn’t know how much.
Knowing what is coming and when, a manual system using CGM and a suitable “controller” App (with added patient food and exercise input) could do an even better job at much less cost. Would it be worth creating an Open Software project for such an App?
David, we agree on a lot of things – like the fact that in most closed loops, meal boluses are still important given the timing of today’s available insulin (which is why you’ll see that it’s a part of the OpenAPS reference design and reflected in the outcomes of the data presented in the poster). And, even an “open loop” system can provide a lot of benefit to many people with diabetes! You should join us over on Gitter to discuss some of these ideas, there’s a few open source apps that are taking on the “open loop” approach, and many of the features we’re building into #OpenAPS (like “eating soon” mode and other elements) are also features that can be used by any person with diabetes, regardless of the way they choose to administer insulin.