As of March 26, 2024, there are more than (n=1)*3,262+ individuals around the world with various types of DIY closed loop implementations. This is solely based on individuals who have self-reported using a form in the community; the total number of users is likely larger than this number, but this provides a minimum estimate of users which confirms estimates that “thousands” of people are using DIY, open source AID systems. This number continues to grow, as does the number of options for various types of DIY closed loops!
We currently estimate this collective DIY community has more than 100,840,000+ real-world “closed loop hours”. (This rough and *very* conservative calculation for estimating loop hours is based on approximately 8 hours per 24 hour period for someone who uses the system overnight; and 20 hours per 24 hour period for someone who may use the system 24/7, to account for any downtime.)
This means #OpenAPS and other DIY closed loop users experience fewer highs, less severe lows, and more “time in range”: most users self-report less of both highs and lows, plus more time in range, AND hbA1c reductions – not to mention the quality of life improvements associated with having a system that can auto-adjust basal rates overnight while they sleep.
It means #OpenAPS users have more peace of mind to sleep at night for everyone in the family.
See below for a variety of self-reported, retrospective, observational, and prospective studies completed over the past few years. Note: in 2022, the first RCT results were presented and then published in NEJM (see below under 2022 for more details).
2016 Self-reported OpenAPS Outcomes Study
A poster with data from the OpenAPS community was presented in June at the 2016 American Diabetes Association Scientific Sessions meeting. You can read this post for full insights from the poster, or these highlights:
While using OpenAPS, self-reported outcome measures (by 18 of the first 40 users) showed:
- median HbA1c dropped from 7.1% to 6.2%
- median percent time in range (80-180 mg/dL) increased from 58% to 81%
- All but one respondent reported some improvement in sleep quality, and 56% reported a large improvement
2018 Outcomes studies
Additional studies have been done, both in the community and by traditional researchers, looking at outcomes from those using DIY closed loop studies. In addition to the 2016 self-reported outcomes study, in 2018 another outcomes study was presented by the community, showing similar results (n=20). Additionally, two other sets of researchers from Italy (n=30) and Korea (n=20; pediatric population) also presented data analyses with similar outcomes. A summary of these studies and their reduction in A1c, time spent in hypo- and hyperglycemia, as well as improvements in time in range, is visualized below.
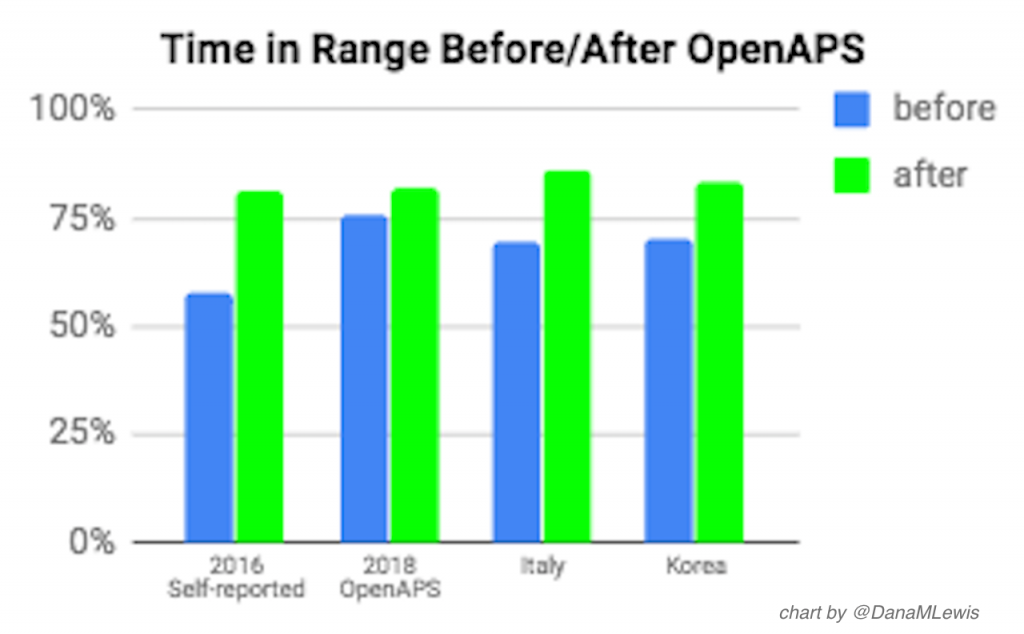
Time in range before and after OpenAPS
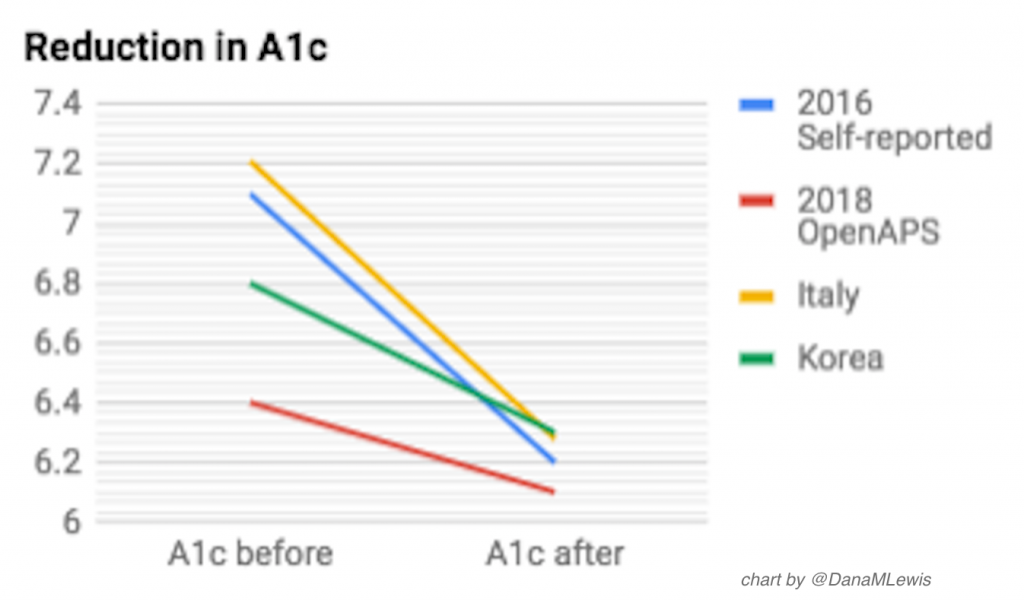
A1c before and after OpenAPS
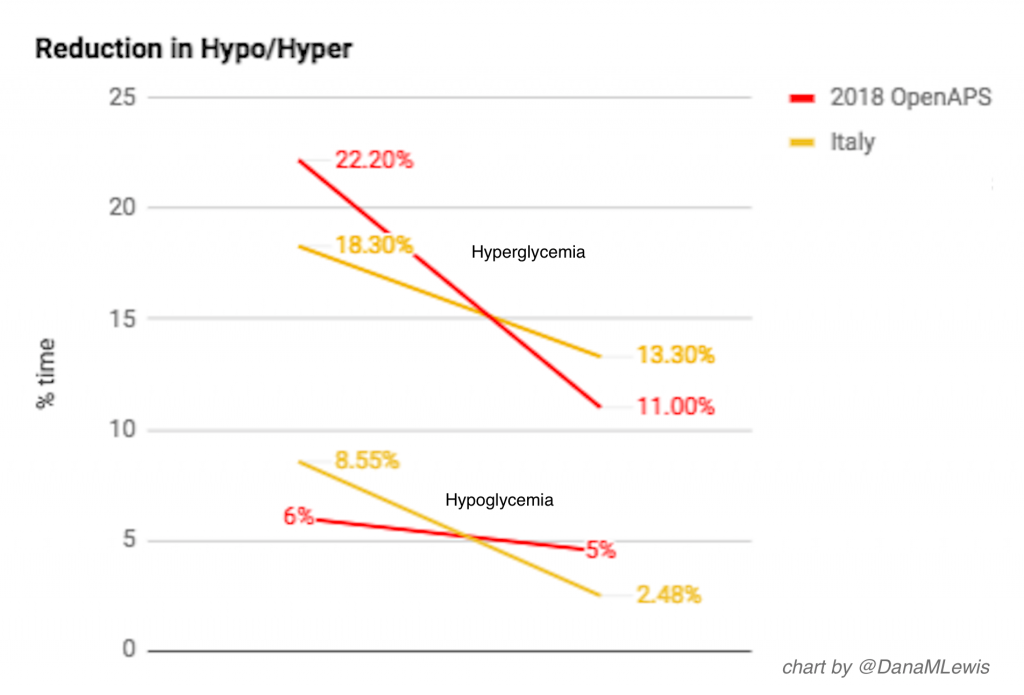
Reduction in hypoglycemia and hyperglycemia after OpenAPS
Also in 2018, Litchman et al. published in JDST a retrospective netnography study over a period of two years, suggesting a correlation between OpenAPS usage and improved A1c and quality of life. See https://doi.org/10.1177/1932296818795705 for the full publication.
2019 studies
- Braune et al published “Real-World Use of Do-it-Yourself Artificial Pancreas Systems in Children and Adolescents: Self-Reported Clinical Outcomes” in JMIR mHealth and uHealth 7.7 (2019): e14087. doi:10.2196/14087
- Melmer et al published a retrospective analysis of n=80 with 19,495 days worth of CGM data. See: “Glycemic Control in Individuals with Type 1 Diabetes Using an Open Source Artificial Pancreas System (OpenAPS)” in Diabetes, Obesity and Metabolism (2019). doi:10.1111/dom.13810
- Toffanin et al published a study using the UVA Padova simulator for in silico safety trials of the OpenAPS algorithm. See “In silico trials of an open-source android-based artificial pancreas: a new paradigm to test safety and efficacy of do-it-yourself systems.” Diabetes Technology and Therapeutics ja (2019). doi:10.1089/dia.2019.0375
- And, Koutsovasilis et al presented a prospective study of the OpenAPS algorithm at EASD in 2019. See: “Clinical evaluation of a closed-loop insulin delivery system on glycaemic control in adults with type 1 diabetes”
2020 studies
- Zabinsky J, Howell H, Ghezavati A, Lewis DM, Nguyen A, Wong J. “Do-It-Yourself Artificial Pancreas Systems for Type 1 Diabetes Reduce Hyperglycemia without Increasing Hypoglycemia”. Diabetes 2020 Jun; 69(Supplement 1): https://doi.org/10.2337/db20-988-P
- Wu, Zekai, et al. “Use of a do-it-yourself artificial pancreas system is associated with better glucose management and higher quality of life among adults with type 1 diabetes.” Therapeutic Advances in Endocrinology and Metabolism 11 (2020). https://doi.org/10.1177/2042018820950146
- Volkova, A, Chernaya, M, Vlasova, K. “Experience of using insulin therapy with the closed loop method among patients with type 1 diabetes mellitus in Russia”. Endocrine Abstracts (2020) 70 AEP329. DOI: 10.1530/endoabs.70.AEP329
- Asarani, N.A.M., Reynolds, A.N., Elbalshy, M. et al. “Efficacy, safety, and user experience of DIY or open-source artificial pancreas systems: a systematic review”. Acta Diabetol (2020). https://doi.org/10.1007/s00592-020-01623-4
2021 studies
- Gawrecki A, Zozulinska-Ziolkiewicz D, Michalak MA, Adamska A, Michalak M, Frackowiak U, Flotynska J, Pietrzak M, Czapla S, Gehr B, Araszkiewicz A. “Safety and glycemic outcomes of do-it-yourself AndroidAPS hybrid closed-loop system in adults with type 1 diabetes”. Plos one. 2021 Apr 5;16(4):e0248965. https://doi.org/10.1371/journal.pone.0248965
- Lal RA, Maikawa CL, Lewis D, Baker SW, Smith AA, Roth GA, Gale EC, Stapleton LM, Mann JL, Yu AC, Correa S. “Full closed loop open‐source algorithm performance comparison in pigs with diabetes”. Clinical and Translational Medicine. 2021 Apr;11(4):e387. https://doi.org/10.1002/ctm2.387
- Jeyaventhan R, Gallen G, Choudhary P, Hussain S. “A Real‐World Study of User Characteristics, Safety and Efficacy of Open‐Source Closed‐Loop Systems and Medtronic 670G”. Diabetes, Obesity and Metabolism. 2021 May 17. https://doi.org/10.1111/dom.14439
- Braune K, Gajewska KA, Thieffry A, Lewis DM, Froment T, O’Donnell S, Speight J, Hendrieckx C, Schipp J, Skinner T, Langstrup H. “Why #WeAreNotWaiting—Motivations and Self-Reported Outcomes Among Users of Open-source Automated Insulin Delivery Systems: Multinational Survey”. Journal of Medical Internet Research. 2021 Jun 7;23(6):e25409. https://doi.org/10.2196/25409
- Knoll, C, et al. “Real‐World Evidence on Clinical Outcomes of People with Type 1 Diabetes Using Open‐Source and Commercial Automated Insulin Dosing Systems: A Systematic Review.” Diabetic Medicine, 2021, https://doi.org/10.1111/dme.14741
2022 studies
- Patel R, Crabtree TS, Taylor N, Langeland L, Gazis T, Mendis B, Wilmot EG, Idris I. “Safety and effectiveness of Do‐It‐Yourself Artificial Pancreas System (DIYAPS) compared with continuous subcutaneous insulin infusions (CSII) in combination with Free Style Libre (FSL) in people with Type 1 diabetes”. Diabetic Medicine. 2022 Jan 11:e14793. https://doi.org/10.1111/dme.14793
- Shahid, A, Lewis DM. “Large-Scale Data Analysis for Glucose Variability Outcomes with Open-Source Automated Insulin Delivery Systems”. Nutrients 2022, 14, 1906. https://doi.org/10.3390/nu14091906
- Amuedo, S, Antequera, M, Azriel, S. “Real-World Use of Do-It-Yourself Artificial Pancreas Systems in Adults with Type 1 Diabetes”. Diabetes 1 June 2022; 71 (Supplement_1): 800–P. https://doi.org/10.2337/db22-800-P
- Burnside M, Lewis D, Crocket H, Wilson R, Williman J, Jefferies C, et al. “The CREATE Trial: Randomized Clinical Trial Comparing Open-Source Automated Insulin Delivery with Sensor Augmented Pump Therapy in Type 1 Diabetes”. Diabetes 1 June 2022; 71 (Supplement_1): 286–OR. https://doi.org/10.2337/db22-286-OR
- Burnside M, Lewis D, Crocket H,et al. Open-Source Automated Insulin Delivery in Type 1 Diabetes. N Engl J Med 2022;387:869-81. DOI:10.1056/NE/Moa2203913
- Shahid, A.; Lewis, D. Large-Scale Data Analysis for Glucose Variability Outcomes with Open-Source Automated Insulin Delivery Systems. Nutrients 2022, 14, 1906. https://doi.org/10.3390/nu14091906
- Müller-Korbsch M, Frühwald L, Kietaibl A. Changes in Ambulatory Glucose Profile in Patients With Type 1 Diabetes Mellitus After Switching From Sensor-Augmented Insulin Pump Therapy to a Do-It-Yourself Artificial Pancreas System: A Retrospective Data Analysis of Real-World Data. Journal of Diabetes Science and Technology. August 2022. doi:10.1177/19322968221114112
2023 studies
- Burnside, M; Lewis, D; Crocket, H; et al. Extended Use of an Open-Source Automated Insulin Delivery System in Children and Adults with Type 1 Diabetes: The 24-Week Continuation Phase Following the CREATE Randomized Controlled Trial. Diabetes Technology & Therapeutics. 2023. https://doi.org/10.1089/dia.2022.0484
- Cooper D, Reinhold B, Shahid A, Lewis DM. Glucose Variability Analysis in Two Large-Scale and Real-World Data Sets of Open-Source Automated Insulin Delivery Systems. Journal of Diabetes Science and Technology. 2023;0(0). doi:10.1177/19322968231198871
- Klimontov V.V., Shishin K.S. Open source automated insulin delivery systems: experience of russian patients. Diabetes mellitus. 2023;26(6):615-618. (In Russ.) https://doi.org/10.14341/DM13033
- Petruzelkova, L., Neuman, V., Plachy, L., Kozak, M., Obermannova, B., Kolouskova, S., Pruhova, S. and Sumnik, Z., 2023. First use of open-source automated insulin delivery Androidaps in full closed-loop scenario: Pancreas4All randomized pilot study. Diabetes Technology & Therapeutics, 25(5), pp.315-323. doi:10.1089/dia.2022.0562
- Nanayakkara N, Sharifi A, Burren D, Elghattis Y, Jayarathna DK, Cohen N. Hybrid Closed Loop Using a Do-It-Yourself Artificial Pancreas System in Adults With Type 1 Diabetes. Journal of Diabetes Science and Technology. 2023;0(0). doi:10.1177/19322968231153882